# Wrap Up: What Happened to the Man who Lost His Breath?
## **How did COVID-19 emerge as a new virus in December 2019?**
Source: [National Institute on Drug Abuse](https://d14rmgtrwzf5a.cloudfront.net/sites/default/files/animated-graphic-2019-ncov.jpg)
* COVID-19 stands for COronaVIrus Disease 2019. Coronavirus is the family of viruses that this new virus belongs to. Other viruses in the coronavirus family include many of the viruses that cause the common cold, Middle East Respiratory Syndrome (MERS), and Severe Acute Respiratory Syndrome (SARS).
* The virus was thought to be transmitted from a bat to a human and has features that allow it to spread well from person-to-person.
* Viruses that spread from animals to humans are called “zoonotic viruses” and include the flu, Ebola, Zika, and HIV.
* Since it is a virus that humans have not been exposed to before, we don’t have immunity to it, which is why so many people around the world are getting sick.
### **How is COVID-19 spread?**
The virus is spread by respiratory droplets, such as when someone with the virus sneezes, coughs, or talks and you breathe it in, or when you touch a surface that a droplet was on and then touch your mouth, nose, or eyes. It is important to know that COVID-19 can infect anyone, regardless of where they’re from or what they look like.
### **How does COVID-19 replicate in the body?**
* COVID-19 uses a receptor we have on the cells that line our mouth, nose, and lungs to get inside our cells.
* Once in the cell, it hijacks the cell’s machinery to replicate and then releases more viruses to go infect other cells.
* The immune system is supposed to recognize these infected cells and kill them so that the virus can’t keep replicating. The older we get, the harder it is for our body to fight infection, which is why we think that older people are more susceptible to severe illness.
### **What are the symptoms of COVID-19?**
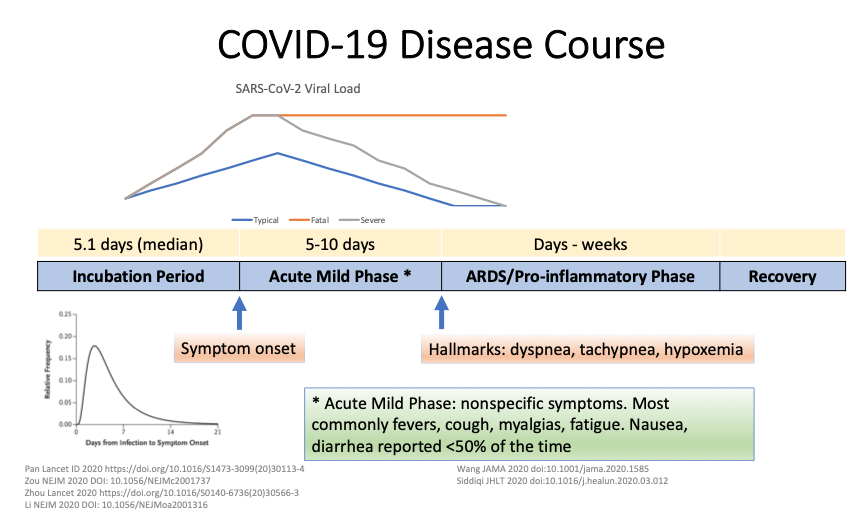
Source: Richterman and Meyerowitz, Partners ID Grand Rounds 3/25/20
* Fever
* Fatigue
* Cough (usually dry cough but can produce mucus/phlegm)
* Loss of appetite
* Myalgias (muscle pains)
* Shortness of breath
* Can be asymptomatic
* Disease can range from asymptomatic to multiorgan failure
### **How do we diagnose COVID-19?**
* Gold standard of diagnosis is the test for COVID-19: RT-PCR, which looks for genetic material from the virus on nasopharyngeal swabs.
* Lab values are highly variable and not useful for making the diagnosis, but we often see low white blood cell count.
* Chest CT typically shows ground glass opacities, consistent with appearance of viral pneumonia - however, chest CT not recommended as screen for COVID-19.
* Lung exam often shows abnormal breath sounds as expected in pneumonia - crackles (faint popping sounds - like popping bubble wrap), wheezing (high-pitched whistling), egophony (more high frequency sounds). These all indicate the presence of fluid and inflammation in the infected lungs.
#### Many people who get COVID-19 show minimal symptoms or have a mild flu-like illness where they can recover at home. What types of people are more susceptible to severe infection that requires hospitalization?
* Elderly - immune system gets weaker as we get older
* Immunocompromised - e.g. on cancer treatment, smokers, people with organ transplants, people with immune deficiencies, people with HIV/AIDS - immune system doesn’t work well to fight off viruses
* People with chronic health problems
* People with lung disease - asthma, COPD
* People with other systemic comorbidities - diabetes, severe obesity, on dialysis for chronic kidney disease, liver disease
* People with a history of smoking/vaping or current smokers - these inhaled agents damage lungs
* People with obesity (those who are overweight)
### **What was happening in our patient’s lungs in part 2 when he suddenly had a really hard time breathing?**
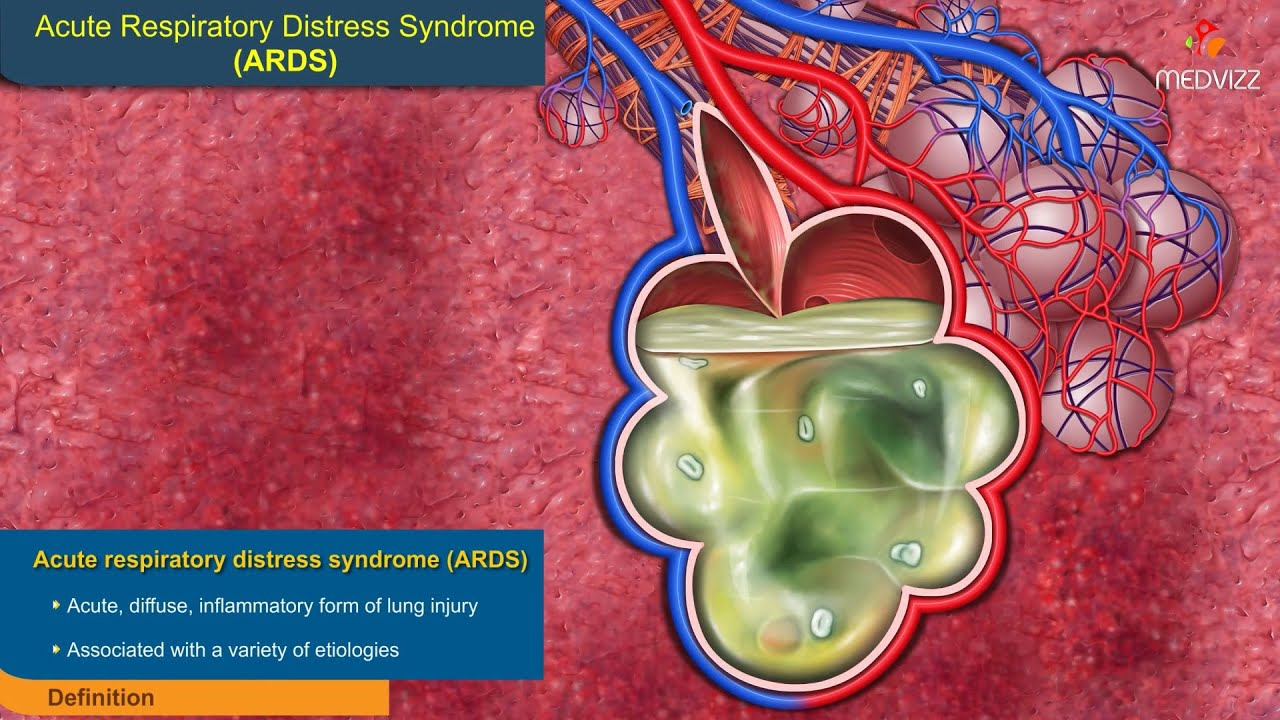
Source: [Medvizz](https://i.ytimg.com/vi/KXw8LXKcmrw/maxresdefault.jpg)
When you have an infection, your body tells your blood vessels to be more leaky so that immune cells can leave the bloodstream to fight infections. However, when your body is fighting off a bad infection, your body can produce too much inflammation and make the vessels too leaky. In Acute Respiratory Distress Syndrome (ARDS), inflammation causes increased leakiness of capillary vessels in the lung, which fills the alveoli and area around the alveoli (the interstitium) with fluid. ARDS is sometimes colloquially referred to as “wet lung” for this reason. When the alveoli are filled with fluid, they cannot fill up with air and your body cannot get oxygen -- which is why it presents as low oxygen saturation and difficulty breathing. ARDS is a medical emergency since the patient is essentially drowning in their own lung tissue.
### **How does a ventilator help a patient with ARDS from COVID-19 recover?**
In ARDS, there is fluid in the alveoli. The ventilator’s PEEP setting helps give extra pressure to push the fluid out of the alveolus so that it can be reabsorbed into the capillary and allow for air exchange.

Source: Created by Jessica Laird
### **What other treatments do we have for COVID-19?**
* Currently we do not have any specific treatments for COVID-19.
* We help treat the specific symptoms each patient is experiencing -- monitoring them for complications, tylenol for fevers, intravenous fluids for hydration, giving oxygen or ventilatory support to patients with respiratory difficulties.
* Many different treatments are being tested for efficacy in patients with COVID-19, but nothing has shown significant promise yet. The medications being tested out are ones that worked against MERS and SARS.
* We are starting to have a few medicines (Remdesivir, dextamethasone) that may help certain people who are sick with coronavirus. Doctors are still studying how effective these medications are.
* Now we have a mRNA vaccine for COVID-19
### **What are we doing as a society to reduce the spread of COVID-19?**
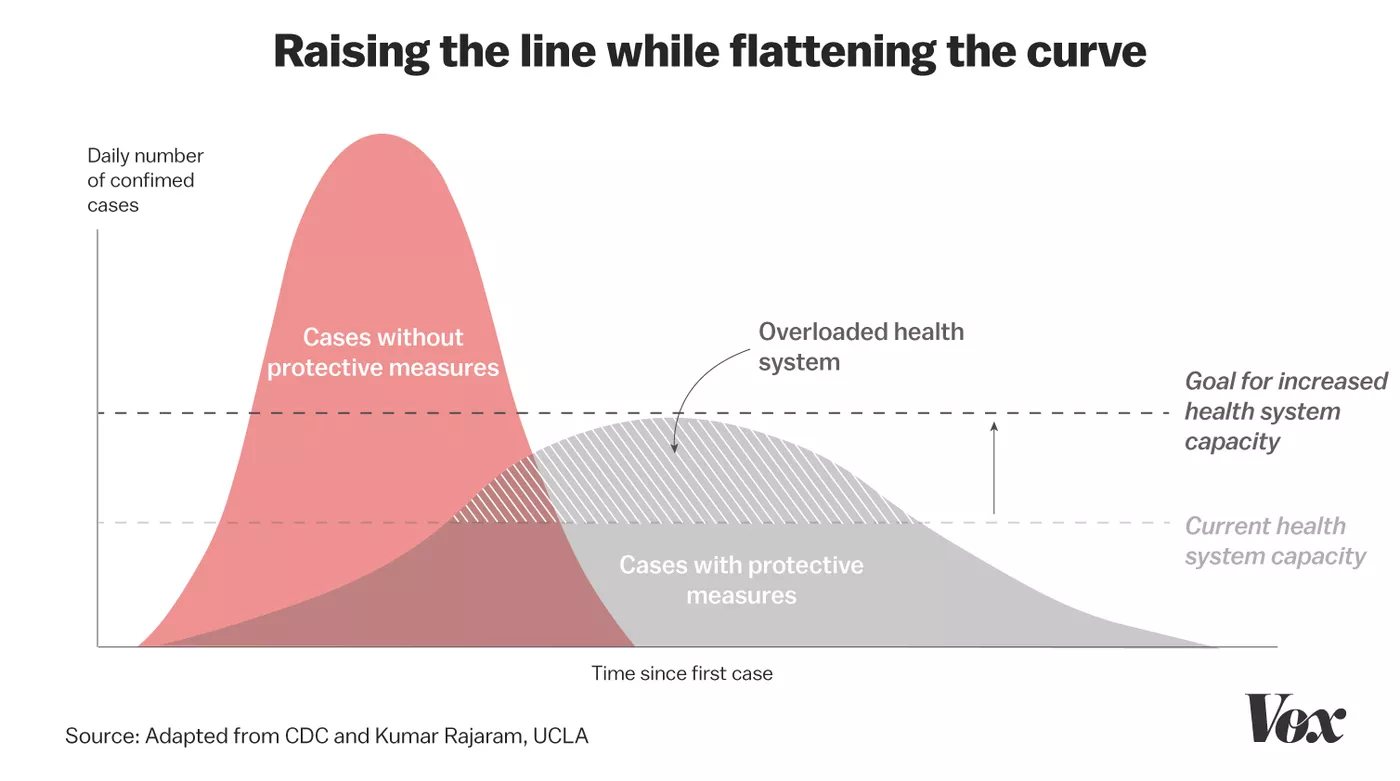
Source: [Vox](https://cdn.vox-cdn.com/thumbor/k-wYSoMv5Ay5VlDXDGBetXICM-A=/1400x0/filters:no_upscale\(\)/cdn.vox-cdn.com/uploads/chorus_asset/file/19874507/flattening_the_curve_2.jpg)
* Contact tracing: Close contacts of a known case are identified, told of exposure, and encouraged or mandated to self-quarantine. Need to be able to test widely and use a lot of time and resources to find the people who may have been exposed.
* Quarantine: Restricts movement of people exposed to contagious disease to monitor for development of disease. This principle is based on the idea that people can be infectious before they become symptomatic.
* Isolation: Separating sick people from those who are not sick to prevent spread of disease.
* Flattening the curve: Slowing the spread of disease in order to limit the number of people who are sick at once. The healthcare system can only treat a limited number of sick patients at once (due to a limited amount of staff and equipment). Slowing the spread of the disease prevents the healthcare system from getting overwhelmed so that it can provide care for those who need it when they need it.
* Physical distancing: Minimizing contact between people in different households can significantly reduce spread of disease through asymptomatic people.
### **What do I need to know? What can I do to help?**

I worked with a group of medical students interested in pediatrics to create this sheet. It and many other fact sheets, including fact sheets in many languages, are available at [https://covid19healthliteracyproject.com/](https://covid19healthliteracyproject.com/#english).
In addition, this [handout from CHU Ste-Justine](https://www.cps.ca/uploads/blog_uploads/Tips_and_tricks_adolescence_-_Ste-Justine_-_ENGLISH.pdf), Montreal, Quebec has great information on how to cope with COVID-19, specifically made for high school and college students.
### **Where can I find accurate information about COVID-19?**
* [World Health Organization (WHO) ](https://www.who.int/emergencies/diseases/novel-coronavirus-2019)
* [Center for Disease Control (CDC)](https://www.cdc.gov/coronavirus/2019-nCoV/index.html)
The most important things we can all do to help include following guidelines of physical distancing as long as they are in place, washing our hands well, keeping in good virtual contact with loved ones (especially those living alone) and taking care of our mental wellness. While it’s good to seek out reliable information and guidance from trusted sources (like the WHO and the CDC), it’s also important to monitor your own emotional wellness. Engaging in activities like journaling, meditating, exercising, yoga, deep breathing, and talking to people you trust about how you are feeling are great ways to care for yourself during this tumultuous time. If you haven't already, proceed to \
the guide on "Caring for Yourself and Others during COVID-19" now:
{% content-ref url="/pages/-M5DTjmJLz7KjlMc5Zoz" %}
[Caring for Yourself and Others during COVID-19](/high-school/covid-19-high-school-and-college-student-curriculum/caring-for-yourself-and-others-during-covid-19.md)
{% endcontent-ref %}
---
# Agent Instructions: Querying This Documentation
If you need additional information that is not directly available in this page, you can query the documentation dynamically by asking a question.
Perform an HTTP GET request on the current page URL with the `ask` query parameter:
```
GET https://kids.covidstudentresponse.org/introduction-simulation-telehealth-and-personal-protective-equipment-ppe/wrap-up-what-happened-to-the-man-who-lost-his-breath.md?ask=
```
The question should be specific, self-contained, and written in natural language.
The response will contain a direct answer to the question and relevant excerpts and sources from the documentation.
Use this mechanism when the answer is not explicitly present in the current page, you need clarification or additional context, or you want to retrieve related documentation sections.